Researcher Spotlight: Professor Helen Roche
Research
- Institutes, Centres & Themes
- Researcher Spotlight
- Researcher Spotlight: Dr Ricardo Segurado - Associate Professor
- Researcher Spotlight: Dr Brona Fullen - Assistant Professor
- Researcher Spotlight: Associate Professor Mary Codd
- Researcher Spotlight: Professor Helen Roche
- Researcher Spotlight: Professor Patricia Fitzpatrick
- Researcher Spotlight: Professor Brian Caulfield
- Researcher Spotlight: Professor Anne Drummond
- Researcher Spotlight: Dr Sinead McMahon
- Researcher Spotlight: Dr Seamus Kelly - Assistant Professor
- Researcher Spotlight: Dr Denise McGrath
- Researcher Spotlight: Dr Clare Corish - Associate Professor
- Researcher Spotlight: Dr Tara Cusack - Associate Professor
- Researcher Spotlight: Professor Cecily Kelleher
- Researcher Spotlight: Dr Olive Lennon - Assistant Professor
- Researcher Spotlight: Dr Celine Murrin - Assistant Professor
- Researcher Spotlight: Dr Carla Perrotta - Assistant Professor
- Researcher Spotlight: Dr Grainne O'Donoghue - Assistant Professor
- Course Spotlight: UCD Professional Masters in Physiotherapy - Dr Cliona O'Sullivan
- Course Spotlight: UCD MSc Clinical Nutrition and Dietetics - Dr Clare Corish
- Researcher Spotlight: Dr Cliona O'Sullivan - Associate Professor
- Researcher Spotlight: Dan Horan - PhD Student
- Undergraduate and Taught Masters Research Ethics Committee
PROFESSOR HELEN ROCHE
UCD School of Public Health, Physiotherapy and Sports Science
UCD Conway Institute
UCD Institute for Food and Health
Improving Public Health with Personalised Nutrition
Nutrigenomics is the study of interactions between genes, diet and health.
Personalised nutrition looks at the complex interaction between nutrients and genes to create tailored diets which complement a person's unique genetic profile.
Professor Helen Roche and her UCD team are some of the world leaders in researching personalised nutrition, particularly around obesity, muscle loss through ageing (sarcopenia) and type 2 diabetes. Now, the team is exploring the relevance of nutrigenomics to other diseases.
They have also produced data around gut bacteria which could be used to develop new food products to lower diabetes risk in certain individuals.
NUTRIMAL is an acronym for Novel Nutritional Solutions for Malnutrition in the Elderly.
Prof Roche and her team are conducting a very large study looking at preventing sarcopenia through different combinations of food. They have found that typically only 30-40% of people will respond to nutritional therapy and are trying to identify alternative effective therapies.
Professor Roche has also recently published a paper with global collaborators examining the interactions of nutrition and genes in 19,005 people.
She is also involved with ImmunoMet, in collaborations with Microbiome Ireland and the Kerry Group and funded by Science Foundation Ireland. The microbiome is a person’s gut bacteria, and it may predispose a person to a greater risk of diseases conditions such as obesity, type 2 diabetes or cardiovascular disease.

Prof Roche and her research team have demonstrated that if you put in a diabetes microbiome and feed a high-fat diet, that individual has a much greater risk and faster acceleration of the diabetes disease. If someone has an obese microbiome and a high high-fat diet, they may be obese but don’t progress down the diabetes disease line as quickly.
Kerry Group have also developed a food compound derived from yeast in collaboration with Prof Roche and colleagues. Feeding that yeast-derived food compound to study participants has been demonstrated to changes the metabolism and gut bacteria into a healthy space, even in those who are diabetic and obese. This cannot only resolve the disease but prevent the pathway to diabetes.
Obesity, type 2 diabetes and sarcopenia are too common. Worldwide obesity has nearly tripled since 1975 and in an ageing society this trigger leads to a much greater prevalence of diabetes and sarcopenia. Recent work now highlights that there is a lot of variability in terms of risk factors and long-term prognosis in these large disease groups.
Prof Roches' research projects are essentially trying to address personalised nutrition and better understand disease risk and non-risk, and also if and how some people will respond or not respond to nutritional interventions. She says;
"Our work shows that typically 40% of people with obesity-related conditions such as diabetes may respond well to nutritional intervention but 60% don’t, despite adhering to a good diet. Therefore if they do not, health professionals have to consider something other treatments, like medical exercise or pharmacological options as a treatment."
Similarly, in the ageing and sarcopenia area, some people at risk of sarcopenia might respond better to weight-bearing exercise rather than nutritional or dietary interventions, such as protein supplementation. Or an individual with osteoporosis may respond better to medications alongside nutrition.
"If we can show how and why diet will work better in some people but not others, then personalised nutrition can be more targeted and potentially more effective along with or instead of pharmacological intervention. Additionally, if health professionals could skip the diet component if they know it is not going to be effective and go straight to the other interventions this would be preferable."
The research team do a lot of work in the obesity, sarcopenia and type 2 diabetes space, and in the future hope to explore potential relevance to obesity obesity-related cancers as nutrition would be one of those components.
Professor Roche thinks it is unethical to be treating people if something is going to work in a certain proportion of the population but not in another. And it is important in the context of health and wellness.
Another consideration is that understanding the molecular biomarkers, which are essentially signatures of nutrition response and non-response, has potential economic impact in terms of biomarker patents and new foods. On the biomarker side, which essentially is a ‘healthy nutrition signature’ that typifies someone at risk of diabetes or sarcopenia and who will respond well to a diet.
In the future, about 5-10 years from now, further health, biotechnology and economic impacts will evolve from understanding the nutritional biomarker signatures.
"In the future people will use technology to measure their glucose, cholesterol or muscle strength using new apps on their phone that are linked to sensors, So if a person eats a food that is supposed to resolve high blood sugar or increase muscle mass or strength the consumer will be able to measure their own response."
Therefore, food companies need to know who to promote to foods too, as in those people who will respond well and get the most benefit from their healthy dietary product.
"The work around the microbiome has patentable data, which could be used in terms of developing new food and drinks products which would be effective in changing the microbiome composition in those at high high-risk of diabetes."
Prof Roche comments that the food and drinks sector is Irelands biggest industry, it’s the biggest employer in Ireland, the biggest export, and the biggest contributor to gross domestic product.
As Ireland exports nearly 40% of food to the UK, and with Brexit, the Irish product industry has to be at the cutting edge of food production, such that products can be exported beyond the UK.
She thinks it is also probable that as alluded to above; soon, there will be consumers that eat a new food shot and then measure their health responses, using some form of wearable technology.
If that product food does not work the way the consumer expects, they could then potentially contest the findings with the food production company based off the negative results they see at home.
Additionally they may then share the good or bad results via social media which may then affect the company share price of the product.
Therefore Personalised Nutrition is a big challenge for the Food and Health Industry. This has far-reaching implications and food companies will be thinking along that line.
Prof Roche comments;
"Not only thinking about their products but also thinking - how can we show that our products work? Customers are looking for and will continue to look for objective measurement tools to show that the product they are purchasing is working."
The process of Professor Roche and colleagues work around nutrigenomics is summarised in the graphic below.
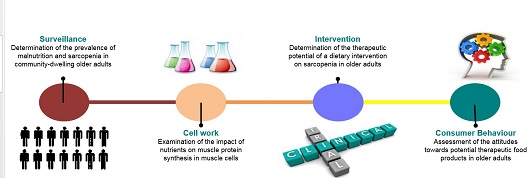
ABOUT THE RESEARCHER

Professor Helen Roche is a Dietitian and head of the Nutrigenomics Research Group in UCD.
(opens in a new window)Helen Roche on Twitter
Helen Roche: Available at (opens in a new window)https://people.ucd.ie/helen.roche.
Associated References
Finucane, O.M., Lyons, C.L., Murphy, A.M., Reynolds, C.M., Klinger, R., Healy, N.P., Cooke, A.A., Coll, R.C., McAllan, L., Nilaweera, K.N. and O’Reilly, M.E. (2015)(opens in a new window)Monounsaturated fatty acid-enriched high-fat diets impede adipose NLRP3 inflammasome–mediated IL-1β secretion and insulin resistance despite obesity. Diabetes, 64(6), pp.2116-2128.
Murphy, C.H. and Roche, H.M. (2018) (opens in a new window)Nutrition and physical activity countermeasures for sarcopenia: Time to get personal?. Nutrition Bulletin, 43(4), pp.374-387.