Genetic Screening of Cancer Cell Lines to Identify New Targeted Treatments
One of the goals of personalised cancer therapeutics is to develop approaches that specifically kill tumour cells without harming healthy cells. A feature of tumour cells that we can exploit is the changes in their DNA that distinguish them from healthy cells.
In the process of becoming cancerous, tumour cells accumulate a wide variety of genetic changes or mutations. Often the same genes, termed driver genes, are mutated again and again in different tumours. Mutations in these driver genes may make the tumour cells uniquely vulnerable to specific drugs. One example of this is the drug Vemurafenib, which targets a mutant form of the BRAF gene, often mutated in melanomas. Vemurafenib specifically kills cells with the mutant form of the BRAFgene, leaving healthy cells alone. Similarly the drug Lynparza can be used to specifically kill ovarian tumour cells with mutations in the BRCA1 or BRCA2 genes.
Major efforts are now underway to identify new targeted treatments that may selectively kill tumour cells harbouring different driver gene mutations. One approach is to screen existing drugs in panels of cancer cell lines to see which drugs kill which cell lines. By connecting this data with genome sequencing in the cell lines it is possible to associate a particular mutation with increased sensitivity to particular drugs. When the drugs involved are approved for clinical use, this may lead to the rapid progression from initial discovery to use in patients, making this a very appealing approach. However, the majority of human genes cannot be inhibited with existing drugs and consequently this approach may miss targets that would be very effective if we developed new drugs for them.
An alternative approach is to use genetic screening to identify genes that different cancer cell lines depend upon for survival. Recently, as part of work I became involved in as a visiting researcher at the Institute of Cancer Research (ICR) in London, I and colleagues from the ICR Gene Function Laboratorypublished a resource that describes how different cancer cell lines depend upon a set of genes known as kinases. Kinases are responsible for transferring information within cells and their functionality is often altered in cancer such that they send the wrong signals. Because of this, and because it is relatively easy to develop drugs to inhibit them, kinases are an especially useful set of genes to study in cancer. Indeed, the majority of existing targeted treatments in cancer inhibit kinases.
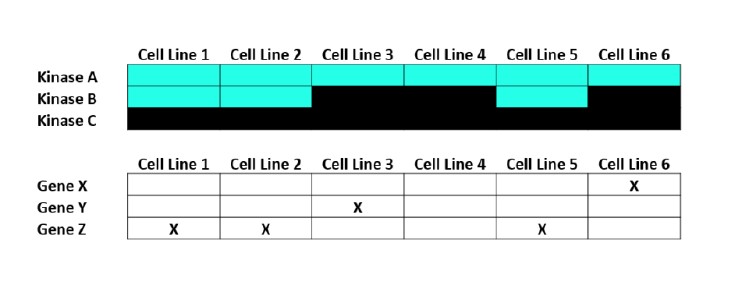
Our team, comprised of experimental and computational biologists, used a technique called RNA interference (RNAi) that allows us to stop specific genes from functioning. We used RNAi to measure how stopping the function of each kinase impacts the growth of over 100 different cell lines. Some kinases, when targeted with RNAi, inhibit the growth of all cell lines suggesting that these genes may be universally important. Others when inhibited appear to cause little or no effect on any cell lines, suggesting that targeting them may have no impact on tumour growth. However, some kinases selectively kill cell lines harbouring particular mutations, suggesting that they may make good starting points for targeted treatments.
In our study we found hundreds of instances where mutation of a driver gene was associated with an increased dependency upon a particular kinase. One example is an apparent dependency of RB1 mutant osteosarcoma cell lines upon a kinase called DYRK1A. Osteosarcomas are a type of bone cancer that primarily impacts children and adolescents, and they frequently harbour mutations in a driver gene called RB1. We found osteosarcoma cell lines with mutations in RB1 were especially sensitive to RNAi inhibition of DYRK1A. This suggests that osteosarcomas harbouring RB1 mutations may be especially sensitive to drugs that inhibit DYRK1A.
It's important to note that this does not mean doctors will start treating osteosarcomas with drugs targeting DYRK1A in the near future - rather it suggests that this may be a promising avenue for further research. A potential first step in this direction would be testing if DYRK1A inhibition kills additional osteosarcoma cell lines harbouring RB1 mutations. Another step would be the identification of drugs that specifically inhibit DYRK1A functionality, while a further possibility would be testing in more realistic models than cell lines (such as mouse models of osteosarcoma). So there is a still lot of work to translate these results from initial discovery to new treatments, but our resource will hopefully speed up the discovery side of the equation.
Further information
Large-Scale Profiling of Kinase Dependencies in Cancer Cell Lines.
Campbell J, Ryan CJ, Brough R, Bajrami I, Pemberton HN, Chong IY, Costa-Cabral S, Frankum J, Gulati A, Holme H, Miller R, Postel-Vinay S, Rafiq R, Wei W, Williamson CT, Quigley DA, Tym J, Al-Lazikani B, Fenton T, Natrajan R, Strauss SJ, Ashworth A, Lord CJ.
Cell Rep. 2016 Mar 15;14(10):2490-501. doi: 10.1016/j.celrep.2016.02.023. Epub 2016 Mar 3.
Study reveals enzymes that cancers depend on to survive
Institute of Cancer Research news
4 Mar 2016

About the Author
Colm Ryan is a Sir Henry Wellcome Postdoctoral Fellow based in Systems Biology Ireland and the Institute of Cancer Research in London. His research aims to improve our understanding of synthetic lethality treatments in cancer therapeutics.

